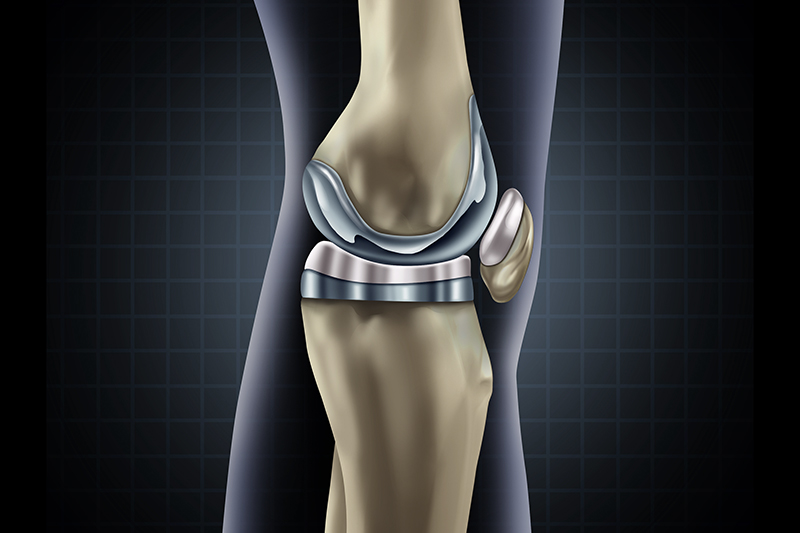
Knee replacement surgery restores a damaged, worn, or diseased knee joint. It is one of the most successful procedures, enabling people to live more active lives free of chronic knee pain. However, a knee replacement may fail for a variety of reasons. When this occurs, your knee can become unstable, painful and swollen. If your knee replacement fails, your doctor may recommend that you have a revision surgery.
A failed knee implant
Although most total knee replacements are successful, over time problems such as implant wear and loosening may require a revision procedure. The revision surgery is the replacement of the previous failed total knee prosthesis with a new prosthesis. It is a complex procedure that requires extensive preoperative planning, specialized implants and tools, prolonged operating time, and mastery of difficult surgical techniques to achieve a good result.
Symptoms of knee replacement failure
Knee pain Swelling Stiffness Mobility issues
Reasons for a revision
1) Non-infected cause
- Implant loosening
- Misalignment: Knee replacement components have to be precisely aligned to work. If they do not line up (deviation of more than three degrees from the mechanical axis), they can wear out too soon.
- Loosening: Faulty components, wear and tear
- Patellar malalignment or instability
- Malalignment of knee (valgus/varus) leads to greater risk of failure
- Patellar dislocation: causing severe knee pain when the patient walks
- Worn out knee joint
- patients who are younger when they undergo the initial knee replacement may outlive the life expectancy of their artificial knee
- Wear of the plastic spacer between the two metal components of the implant
- In some cases, tiny particles that wear off the plastic spacer accumulates around the joint and are attacked by the body’s immune system (giant cell). This immune response also attacks the healthy bone around the implant, leading to a condition called osteolysis (bone defect). This causes the bone around the implant to deteriorate, making the implant loose or unstable.
- High-impact activities, excessive body weight
- Stiffness: Sometimes a total knee replacement may not help you achieve the range of motion that is needed to perform everyday activities. This may happen if excessive scar tissue has built up around the knee joint. If extensive scar tissue or the position of the components in your knee is limiting your range of motion, revision surgery may be needed.
- Material of an implant: The implants are typically secured to the bone with cement. Good quality implants retain their strength and shape for a long time.
- Wrong-sided implant use: unlikely to happen
- Fracture: A periprosthetic fracture is a broken bone that occurs around the components of a total knee replacement. These fractures are most often the result of a fall, and usually require revision surgery.
2) Infection: Infection is a potential complication in any surgical procedure, including total knee replacement surgery. Infections may occur after the surgery or years later.
- Early infection: might be caused by intraoperative infection. This leads to swelling, inflammation, and pus formation.
- Late infection that occurs years after surgery: Bacteria might enter a person’s body through the wound or from an infection in other organs. If bacteria reach a person’s new artificial knee joint, they may multiply and cause an infection. An infection that goes beyond the superficial tissues and gain deep access to the artificial joint almost always requires surgical treatment. Signs and symptoms of an infected joint replacement includes: pain, swelling, warmth, and redness.
Revision surgery for infection
Revision for infection can be done in many ways, depending on the degree of infection and how long the infection has been present. Debridement can be done in some cases where the bacteria can be washed out, the plastic spacer can be exchanged, and the metal implants can be left in place. In other cases, the implant must be completely removed and temporary cement spacer is placed that is treated with antibiotics to fight the infection. When the infection has been cleared, your doctor will perform a second surgery to insert a new prosthesis.
In some cases, there may be significant bone loss around the knee due to the infection. The surgeon might install metal pieces to reinforce the bone for the implant or fasten the implant to the bone. A revision requires the surgeon to use a specialized prosthetic device.
Prevention of infection after knee replacement surgery
An infection after knee replacement surgery can be a serious complication. Although infections occur in only a small percentage of patients, it can prolong or limit full recovery. Below is what you need to know to help protect your new knee so you can enjoy its mobility for years to come.
- Avoid getting wounds
- Avoid getting animal bites
- Keep your house clean
- Avoid water-contact to the surgical wound
- Stop smoking
- Consult your dentist before any dental procedures as antibiotics should be taken prior to the procedures. This is to protect the implants from bacteria that might enter the bloodstream during the dental procedure.
- In patients with diabetes, maintain healthy blood sugar level.
Finding the right surgeon, having a surgery in a hospital with surgical hygiene standards, and using the best quality implants, will help ensure you have a successful surgery and recovery.
At Bangkok hip and knee center, we ensure that every patient receives the best standard of care according to JCI (Joint Commission International) standard. Our highly experienced surgeons will discuss with you and your family in order to determine which surgical technique and prosthesis type will be the most effective for you. After your surgery, we will contact you periodically to see how your knee replacement is doing.